Article: Scaling Community Attitudes Toward the Mentally Ill
Scaling Community Attitudes Toward the Mentally III
by S. Martin Taylor and Michael J. Dear
Abstract
The measurement of public attitudes toward the mentally ill has taken on new significance since the introduction of community-based mental health care. Previous attitude scales have been constructed and applied primarily in a professional context. This article discusses the development and application of a new set of four scales explicitly designed to measure community attitudes toward the mentally ill. The scales represent dimensions included in previous instruments, specifically, authoritarianism, benevolence, social restrictiveness, and community mental health ideology, but are expressed in terms of an almost completely new set of items that emphasize community contact with the mentally ill and mental health facilities. Data from a study of community attitudes about neighborhood mental health facilities in Toronto are used to test the internal and external validity of the scales. Results of the analysis provide strong support for the validity of the scales and demonstrate their usefulness as explanatory and predictive variables for studying community response to mental health facilities.
In both America and Canada, the move toward community-based mental health care has caused extensive neighborhood opposition. The media often seem to delight in reporting the negative aspects of community care, such as erratic client behavior or residents’ fear of property value decline. Geographical interest in this topic stems from two sources: first, because citizen opposition can block the siting of a mental health facility, and thereby upset the pattern of client accessibility to a decentralized service system; and secondly, because proximity to mental health centers apparently intensifies opposition, leading to spatial variation in community cognition and perception of facilities.
The purpose of this article is to provide an instrument for the systematic description of community attitudes toward the mentally ill. Previous research has suggested that the social reintegration of ex-psychiatric patients depends crucially upon their acceptance (or rejection) by the host community. Accordingly, we wish to develop scales to measure Community Attitudes Toward the Mentally 111, which will aid in the assessment and prediction of the host community’s reactions. In order to achieve its purpose, the article first reviews existing approaches to the study of attitudes toward the mentally ill. Secondly, the sample frame and database for this study are briefly outlined. Thirdly, the development of the scales is described, and their validity and utility in predicting community reaction are demonstrated. Finally, some comments on the future applications of the scales are offered.
Existing Studies of Attitudes Toward the Mentally III
Geographical interest in mental health care delivery has expanded rapidly during the past decade. Although Smith (1977) has outlined the broad areas of concern in this field, research efforts are only now becoming more coordinated and purposeful. Five themes seem to be gaining prominence in the geographic literature:
- Descriptions of the geographical incidence of mental illness, and its ecological correlates (e.g., Giggs 1973 and Miller 1974).
- Studies in the utilization and accessibility of mental health services (Dear 1977a; Holton, Krame, and New 1973; Smith 1976; Joseph 1979).
- Follow-up studies of the aftercare problems of patients discharged from psychiatric hospitals (Smith 1975; Wolpert and Wolpert 1976; Dear 1977b).
- Analyses of neighborhood opposition to the location of community mental health facilities (Wolpert, Dear, and Crawford 1975; Boeckh, Dear, and Taylor 1980).
- Structural analyses of the community support system for the mentally disabled and other service-dependent populations (Gonen 1977; White 1979; Wolpert 1978; Wolch 1979).
The approach taken in this article derives from the fourth of these themes, but also integrates two other research themes from the psychiatric literature. The first is the substantive documentation of attitudes toward the mentally ill; and the second is the methodological literature on attitude measurement. Because both these fields have been extensively reviewed elsewhere, our purpose here is merely to indicate the major antecedents of our approach.
In the first instance, our work is indebted to the major synthesis on attitudinal research provided by Rabkin (see, for example, Rabkin 1974). She has recorded the increasing volume of research since 1945 on community attitudes, and has recently warned that the steady improvement in community attitudes may have reached a “plateau,” and that current trends in deinstitutionalization may threaten a decline in acceptance (Rabkin 1980). Closely related to this work is the research of Segal and his associates into the dimensions of accepting and rejecting host communities. In an extensive series of reports, Segal has suggested that the reintegration of the mentally ill is closely linked to the characteristics of the host community, of the facility itself, and of its residents (Segal and Aviram 1978). Facilities with the highest level of integration tend to be in neighborhoods with low social cohesion (e.g., downtown areas, with a highly transient population). On the other hand, social integration tends to be lower in highly cohesive neighborhoods (e.g., suburban single-family subdivisions), which tend to close ranks against the incursion of the mentally ill (Trute and Segal 1976).
Against this background of acceptance or rejection and integration or exclusion, we searched a second literature in order to develop a scaling instrument for community attitudes. While there existed several different scaling instruments for measuring professional attitudes toward the mentally ill, very little effort appears to have been made to develop such instruments for assessing community attitudes. Accordingly, we used the two most comprehensive and best-validated of existing scales, the Opinions about Mental Illness (OMI) and Community Mental Health Ideology (CMHI) scales, and adapted them to develop our Community Attitudes Toward the Mentally III (CAMI) scales.
The OMI scales were originally developed in a study of the attitudes of hospital personnel toward mental illness (Cohen and Struenin’g 1962). The OMI comprises five Likert scales that were empirically derived from factor analysis of a pool of 100 opinion statements. The statement pool was compiled primarily to reflect a range of sentiments about mental illness and the mentally ill, but it also drew upon existing scales such as the Custodial Mental Illness Ideology Scale (Gilbert and Levinson 1956), the California F scale (Adorno et al. 1950), and Nunnally’s (1961) multiple item scale. The five OMI scales were labeled as follows: authoritarianism, reflecting a view of the mentally ill as an inferior class requiring coercive handling; benevolence, a paternalistic, sympathetic view of patients based on humanistic and religious principles; mental hygiene ideology, a medical model view of mental illness as an illness like any other; social restrictiveness, viewing the mentally ill as a threat to society; and interpersonal etiology, reflecting a belief that mental illness arises from stresses in interpersonal experience.
Baker and Schulberg (1967) developed a multiple item scale designed specifically to measure an individual’s commitment to a community mental health ideology. The Community Mental Health Ideology (CMHI) scale comprises 38 opinion statements expressing three different aspects of the basic ideology. The conceptual categories focus on characteristics of the total population, rather than merely those seeking psychiatric help; primary prevention, including efforts via environmental intervention; and total community involvement in working with a variety of community resources to assist patients. The scale has been shown to discriminate effectively between groups known to be highly oriented toward this ideology and random samples of mental health professionals.
The OMI and CMHI scales were the basis for measuring attitudes toward the mentally ill in the present study. They were substantially revised with the dual objectives of (1) emphasizing community rather than professional attitudes toward the mentally ill, and (2) reducing the total number of items. Before proceeding with the development of the CAMI scales, we will outline the empirical framework of our study.
A Survey of Community Attitudes in Metropolitan Toronto
The major purpose of our study was to analyze the basis for community opposition to community mental health facilities, with the twin goals of determining the characteristics of “acceptor” and “rejector” neighborhoods and of developing planning guidelines for locating those facilities (Dear and Taylor 1979). Data on attitudes and other resident characteristics were obtained in 1978 by a questionnaire survey of residents in Metropolitan Toronto. A random sample was selected from the total population stratified by three levels of socioeconomic status (high, medium, and low) and two levels of residential location (city and suburb). Separate samples were drawn from areas with and without existing community mental health facilities. The total sample was 1,090 households, 706 from areas without a facility and 384 from areas having a facility. Three types of facility were included in the with-facility sample: outpatient units, group homes, and social-therapeutic (drop-in) centers.
The questionnaire was introduced as a survey of attitudes toward community services; mental health facilities were not mentioned at the outset, and the first three questions asked for general opinions. Subsequent questions elicited information on awareness of neighborhood mental health facilities; attitudes toward the mentally ill (using the CAMI scales); various perceptual, attitudinal, and behavioral reactions to facilities; and personal characteristics. Three parts of this questionnaire are relevant here. First, all 1,090 respondents completed the CAMI scaling instrument. Secondly, they were asked to indicate the desirability of having a potential facility within three different distance zones from their residence: within 1 block; 2-6 blocks; and 6-12 blocks. Respondent ratings were measured on a 9-point labeled scale ranging from “extremely desirable” (1) to “extremely undesirable” (9), with the midpoint (5) as “neutral.” The behavioral response of respondents to the introduction of a facility into their neighborhood was also determined. Finally, all those respondents who were aware of any facility in their neighborhood (n = 132, even though 384 respondents were selected because they lived within one-quarter of a mile of a facility) were asked if they were in favor of, opposed to, or indifferent toward it. Standard socioeconomic and demographic data were also collected for each respondent.
It is important to point out that highly specific labels were devised for use in the survey. Community mental health facilities were defined for the respondent as including
Outpatient clinics, drop-in centers, and group homes which are situated in residential neighborhoods and serve the local community. Mental health facilities which are part of a major hospital are NOT included.
A similar precision was introduced in the definition of the mentally ill, who were characterized as
People needing treatment for mental disorders but who are capable of independent living outside a hospital.
This definition was used to emphasize our focus on the nonhospitalized patient and to reflect the general competence level of users of community mental health facilities in the Toronto area.
Development of the CAMI Scales
Scale Selection. Two related objectives directed the development of scales to measure community attitudes toward the mentally ill. The first was to construct an instrument able to discriminate between those individuals who accept and those who reject the mentally ill in their community. The second was to develop scales to predict and explain community reactions to local facilities serving the needs of the mentally ill. Previous research, as already discussed, shows that attitudes toward mental illness are multidimensional. Given our objectives, it did not seem necessary to construct scales to measure all possible dimensions but rather to focus on those dimensions that are the most strongly evaluative and hence best discriminate between those positively and negatively disposed toward the mentally ill and mental health facilities. To this end, we identified three of the OMI scales (authoritarianism, benevolence, and social restrictiveness) and the CMHI as the most useful existing scales for our purposes.
These four scales in their original form were not appropriate for our Toronto research for two reasons. First, the scales were developed with professionals in mind as the potential respondents. It was therefore necessary to modify them for use in a general population survey. Second, for some of the scales, the number of items was excessive for use in a community survey—particularly when, as in our case, many questions besides attitudes toward mental illness were to be included in the questionnaire. Scale construction for the Toronto study therefore essentially involved developing shortened and revised versions of the original scales to emphasize community rather than professional attitudes toward the mentally ill.
Item Pool. The item pool for pretest purposes comprised 40 statements, 10 for each of the 4 scales. Only 7 of the 40 came from the original OMI and CMHI scales: three for authoritarianism, two for benevolence and social restrictiveness, and none for community mental health ideology. Four additional authoritarianism items came from the Custodial Mental Illness Ideology Scale (CMI) developed by Gilbert and Levinson (1956). For the three OMI scales, the new statements do not alter significantly the content domains of the scales as originally conceived by Cohen and Struening (1962). Their effect is to emphasize those facets of the content domains which impinge most directly on community contact with the mentally ill. For the CMHI scale, the revisions are more fundamental because the original statements were clearly intended for application in a professional context, and hence a completely new set of statements was required for community-based research. These new statements shift the focus of the scale from the professional’s adherence to the general principle of community mental health, as emphasized in the Baker and Schulberg scale, to the acceptance by the general population of mental health services and clients in the community. The themes expressed in the new scales are summarized in the following descriptions.
Sentiments embedded in the authoritarianism statements were: the need to hospitalize the mentally ill (i.e., As soon as a person shows signs of mental disturbance, he should be hospitalized); the difference between the mentally ill and normal people (e.g., There is something about the mentally ill that makes it easy to tell them from normal people); the importance of custodial care (e.g., Mental patients need the same kind of control and discipline as an untrained child); and the cause of mental illness (e.g., The mentally ill are not to blame for their problems). For benevolence, the sentiments were: the responsibility of society for the mentally ill (e.g., More tax money should be spent on the care and treatment of the mentally ill); the need for sympathetic, kindly attitudes (e.g., The mentally ill have for too long been the subject of ridicule); willingness to become personally involved (e.g., It is best to avoid anyone who has mental problems); and anticustodial feelings (e.g., Our mental hospitals seem more like prisons than like places where the mentally ill can be cared for).
The social restrictiveness statements tapped the following themes: the dangerousness of the mentally ill (e.g., The mentally ill are a danger to themselves and those around them); maintaining social distance (e.g., A woman would be foolish to marry a man who has suffered from mental illness, even though he seems fully recovered); lack of responsibility (e.g., The mentally ill are very unpredictable and should not be given any responsibility); and the normality of the mentally ill (e.g., Many people who have never had psychiatric treatment have more serious mental problems than many mental patients). For the CMHI scale, statements expressed these sentiments: the therapeutic value of the community (e.g., The best therapy for many mental patients is to be part of a normal community); the impact of mental health facilities on residential neighborhoods (e.g., Locating mental health facilities in a residential area downgrades the neighborhood); the danger to local residents posed by the mentally ill (e.g., It is frightening to think of people with mental problems living in residential neighborhoods); and acceptance of the principle of deinstitutionalized care (e.g., Mental hospitals have a very limited role to play in a civilized society).
Five of the 10 statements on each scale expressed a positive sentiment with reference to the underlying concept, and the other five were negatively worded. For example for the authoritarianism scale, five statements expressed a pro-authoritarian sentiment, and five were anti-authoritarian. The response format for each statement was the standard Likert 5-point labeled scale: strongly agree/ agree/neutral/disagree/strongly disagree. The statements were sequenced in 10 sets of 4, and within each set, the statements were ordered by scale—authoritarianism, benevolence, social restrictiveness, and community mental health ideology. The aim of this sequencing was to minimize possibilities of response set bias.
Pretest Results. Two separate pretests were conducted to assess the reliability and validity of the statements and scales. The first was based on a group of first year undergraduate students in urban geography (n = 321) at McMaster University and the second on the respondents (n = 54) in a field pretest conducted by the York University Survey Research Centre. For both sets of data, item-total correlations and alpha coefficients were calculated as measures of statement and scale reliability (Nunnally 1967).
When the results from both pretest samples (table 1) are considered, the alpha coefficients for all four scales are above .50, which can be regarded as a satisfactory (though modest) level of reliability in the early stages of scale construction. The coefficients are notably higher for the McMaster student group for three of the scales (except authoritarianism), which have relatively strong alphas above .70.
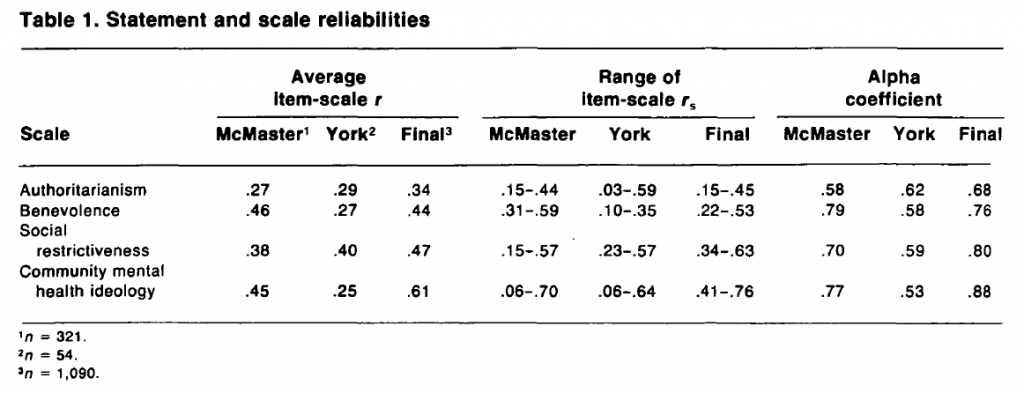
Although the scales are in general satisfactory, inspection of the statement-scale correlations shows a number of statements that make very little contribution to their parent scale. These statements were replaced by statements expressing similar sentiments to those contained in statements more strongly correlated with total scale scores. In addition, two statements on the social restrictiveness scale were replaced to eliminate unnecessary repetition.
Statement and Scale Reliability and Validity for Final Data. The same statistics were calculated to test the reliability and validity of the revised scales using the full Toronto data set (n = 1,090). The alpha coefficients (table 1) are in all cases but one higher than the pretest values, the one exception being on the benevolence scale where the coefficient for the final scale is marginally lower than for the McMaster pretest. Three of the four scales have high reliability: CMHI (a = .88), social restrictiveness (a = .80) and benevolence (a = .76). The coefficient for authoritarianism (a = .68), though lower, is still satisfactory. These increases in the alpha values reflect the general strengthening of the item-total correlation for statements retained from the pretest, and the improvement due to the replacement of the statements shown to be weak in the pretest results.
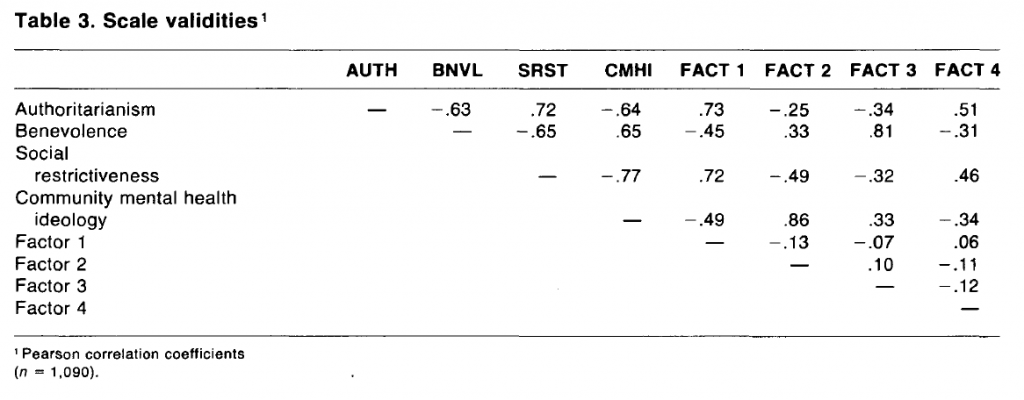
The construct validity of the final scales was assessed by testing their empirical reproducibility using factor analysis. A four-factor orthogonal solution accounting for 42 percent of the variance was obtained (table 2). Factor scores were calculated and correlated with the raw scores on the four a priori scales. The matrix of correlations among the a priori and factor scales (table 3) is revealing in two respects. First, it shows a high degree of intercorrelation among the a priori scales. The lowest correlation is -.63 between authoritarianism and benevolence, and the highest is -.77 between social restrictiveness and CMHI. These coefficients can in part be compared with those reported in previous studies using the OMI (Fracchia et al. 1972). In general, the correlations in this case are higher, possibly reflecting the fact that the distinctions between the scales are not so clear to the general population as they are to the professionals who were respondents in the earlier studies. More importantly, the difference may also reflect the revisions made to the scales for this study.
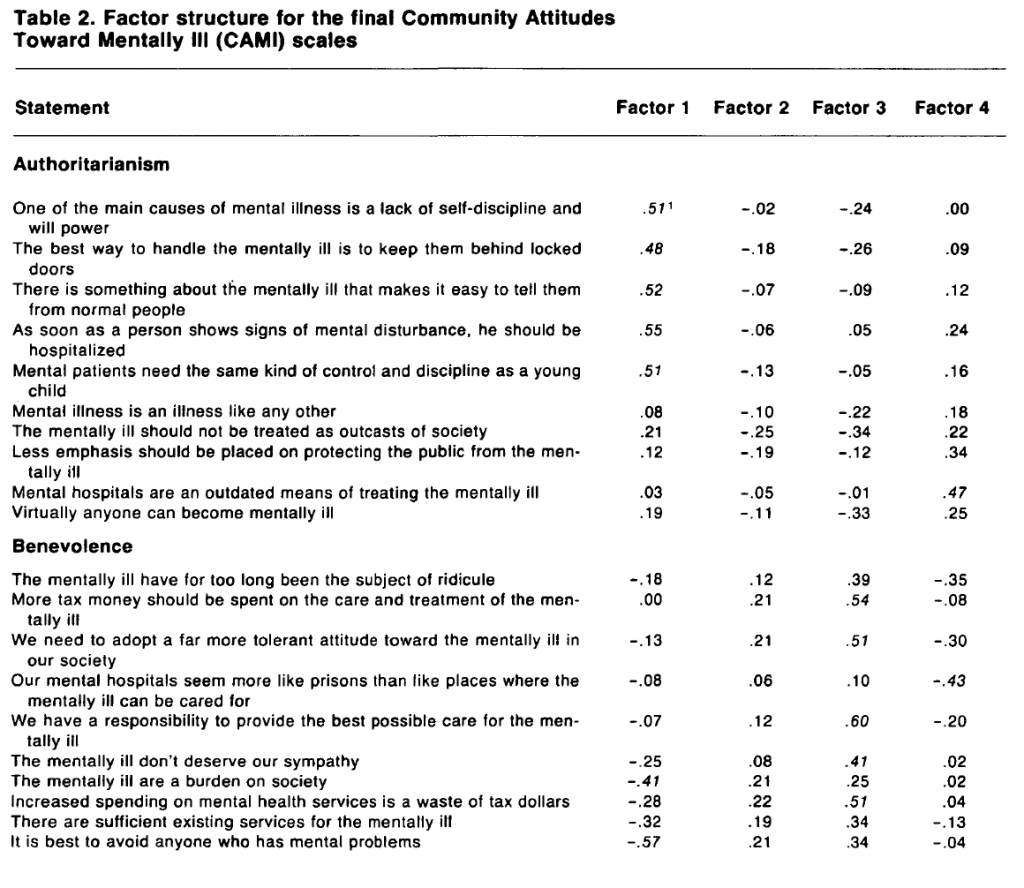
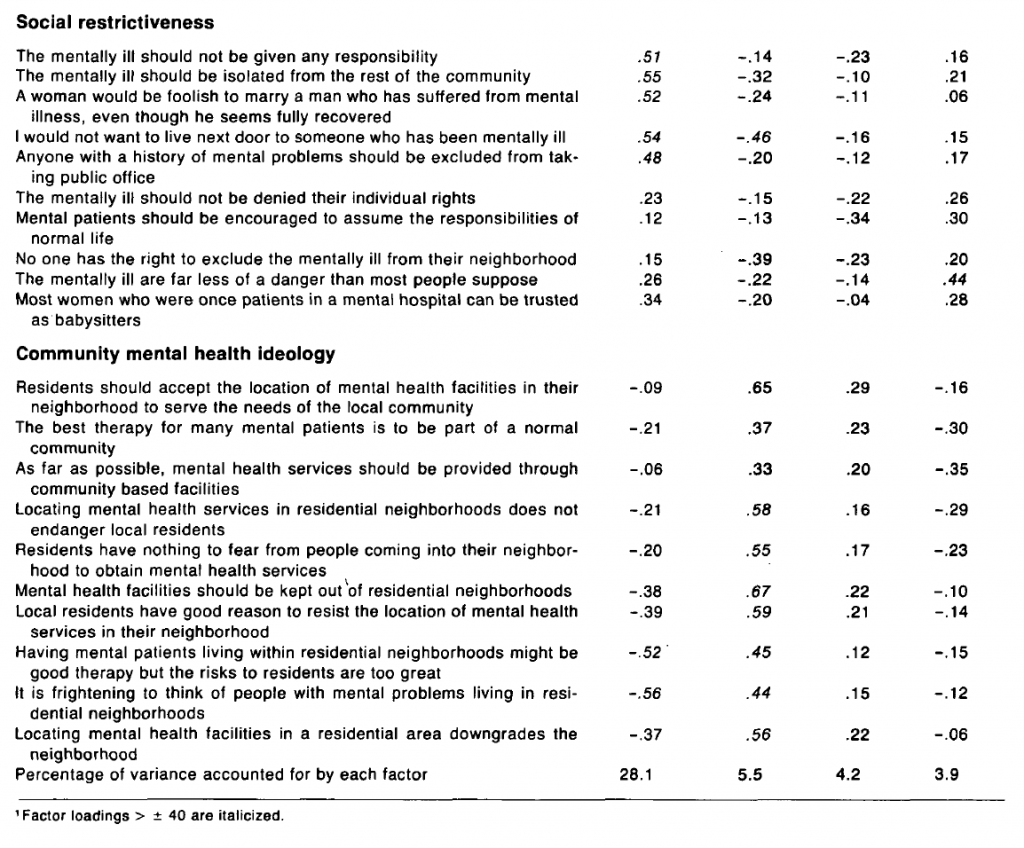
The correlation matrix (table 3) shows secondly a reasonable degree of correspondence between the a priori and factor scales—the desired result from a constant validity standpoint. The CMHI scale is strongly identified with the second factor (r = .86), and the benevolence scale is almost as strongly identified with the third factor (r = .81). Authoritarianism and social restrictiveness are approximately equally correlated with the first factor and, to a lesser extent, with the fourth factor. This provides some evidence that these two scales perhaps represent a single dimension. They are treated separately, however, in the subsequent analyses. The remaining coefficients in the lower right of the matrix show the low correlation among the factor scales. This is an artifact of the algorithm, which forces independence between the factors within an orthogonal solution.

Correlates of Attitudes Toward the Mentally III
The theoretical framework for the Toronto study (Dear and Taylor 1979, chapter 2) is that attitudes toward the mentally ill are a function of a combination of personal characteristics including socioeconomic status, life cycle state, and personal beliefs and values. Existing research on attitudes toward the mentally ill provides some support for the importance of these factors (see Rabkin 1974). The same theoretical framework shows that attitudes toward the mentally ill are the major influence on reactions to mental health facilities. The construct and predictive validity of the attitude scales within this theoretical framework can therefore be examined by analyzing their relationship with, on the one hand, various personal characteristics and, on the other, measures of response to mental health facilities.
Personal Characteristics and Attitudes Toward the Mentally Ill. Three subsets of personal characteristics were distinguished for this analysis: demographic, socioeconomic, and belief variables. Demographic characteristics were measured by four variables: sex, age, marital status, and number of children in three age groups (under 6, 6 to 18, and over 18). Socioeconomic status was measured in conventional terms by educational level, occupational status (both respondent and head of household) and household income, and in addition, by tenure status. Personal beliefs and values were not measured directly. A proxy measure is included in terms of church attendance and denominational affiliation. Also included as a factor affecting beliefs and attitudes toward the mentally ill is a measure of familiarity with mental illness based on whether the respondent or his/her friends or relatives had ever used mental health services of any kind.
The variables used in the analysis represent different levels of measurement—nominal, ordinal, and interval/ratio. The specific measurement properties of the paired combination of variables determine the statistical test used. The CAMI scales are assumed to have interval properties. Tests that relate attitudes to population characteristics with nominal properties are based on a difference of means test (t test) where the characteristic has two categories (e.g., sex), and a one-way analysis of variance (F test) where there are more than two categories (e.g., marital status). Relationships between population characteristics measured on an ordinal scale (e.g., household income) and attitudes toward the mentally ill are tested i by nonparametric correlation (Kendall’s tau). Finally, relationships involving characteristics with interval properties (e.g., age) are tested by parametric correlation (Pearson’s r).
Five of the six demographic variables examined show relatively strong relationships with the four attitude scales, the exception being number of children over 18 (table 4). Consistent with previous studies, older residents report less sympathetic attitudes toward the mentally ill. This pattern occurs for all four scales. Older respondents in the Toronto sample are in general more authoritarian, less benevolent, more socially restrictive, and less community mental health oriented in their views.
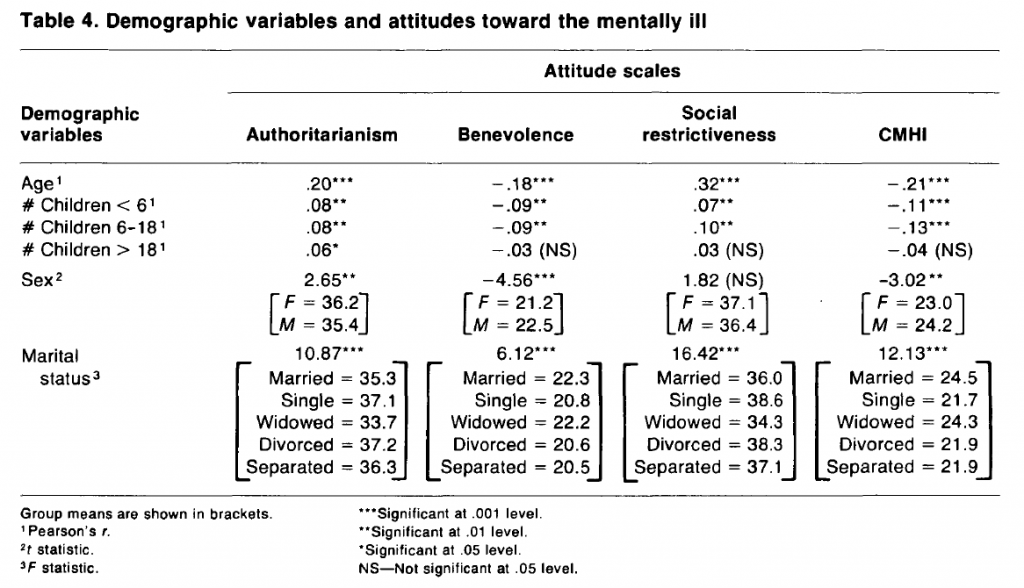
Stronger effects for sex are found for these data than for results reported in previous studies. The direction of the effect shows more sympathetic attitudes among female respondents. This emerges on three of the four scales. No significant difference occurs for social restrictiveness.
Highly significant differences are found among marital status groups on all four scales. Examination of the group mean on each scale reveals the pattern of the effect. A basic distinction emerges between the married and widowed groups and those single, separated, or divorced—the former expressing the less sympathetic attitudes on each of the four scales. These differences in part reflect the age variation already observed and the effects of number and ages of children.
The number of children under 6 years and the number between 5 and 18 years show very similar effects, the latter being marginally stronger. In both cases, respondents with children in these age groups are generally more authoritarian and socially restrictive and correspondingly less benevolent and community mental health oriented. The lack of significant effects for number of children over 18 supports the expectation that parents with older families will have fewer concerns about the mentally ill and their children’s possible contact with them.
Taken together, these results indicate that the effects of demographic characteristics on attitudes toward the mentally ill are both statistically significant and consistent in their direction. The variables included here, excepting sex, represent in combination a measure of life-cycle status. The conclusion is therefore that attitudes toward the mentally ill vary significantly by life-cycle stage.
Four of the five socioeconomic measures show strong and consistent relationships with the attitude scales, the exception being household income (table 5). The observed direction of the relationships confirms previous findings: more sympathetic attitudes are characteristic of higher status residents. This conclusion applies when status is measured in either educational or occupational terms, though the relationships are somewhat stronger for the education variable. Relationships with income, the third conventional measure of socioeconomic status, are weaker and for two scales, benevolence and CMHI, are not significant. This finding indicates that household income varies somewhat differently within the population than does education or occupation and that income is the least effective as a discriminator of attitudes toward the mentally ill.
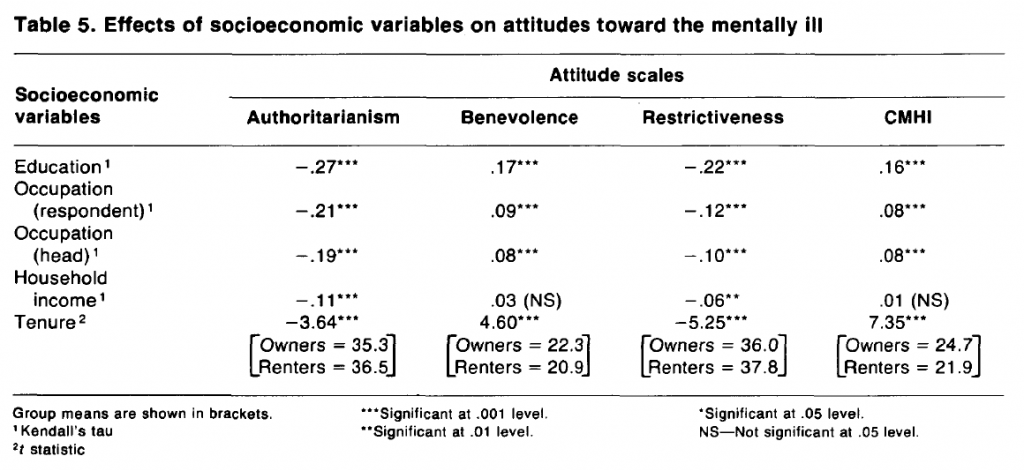
The significant effect of tenure status confirms the expectation that owners generally hold less sympathetic attitudes than renters, possibly reflecting their greater vested interest in protecting their daily life environment.
Within the subset of belief variables, church attendance and familiarity with mental health care show significant relationships with all four attitude scales (table 6). Religious denomination has a significant effect on only the authoritarianism and benevolence scales. The direction of the effect for church attendance is that regular attenders are, on average, less sympathetic in their views, tending to be more authoritarian and socially restrictive and less benevolent and community mental health oriented. As could be expected, regular attenders in general hold more conservative views. Among attenders, however, there are significant denominational differences for two of the scales. Of the 13 major denominational groups distinguished in the survey, the Pentecostal and Greek Orthodox groups emerge as the most authoritarian in contrast to the Baptists and Salvation Army, who expressed the least authoritarian views. Correspondingly, the Baptist, together with United Church, adherents held the most benevolent attitudes, again in contrast to the least benevolent views of the Pentecostal and Greek Orthodox members.
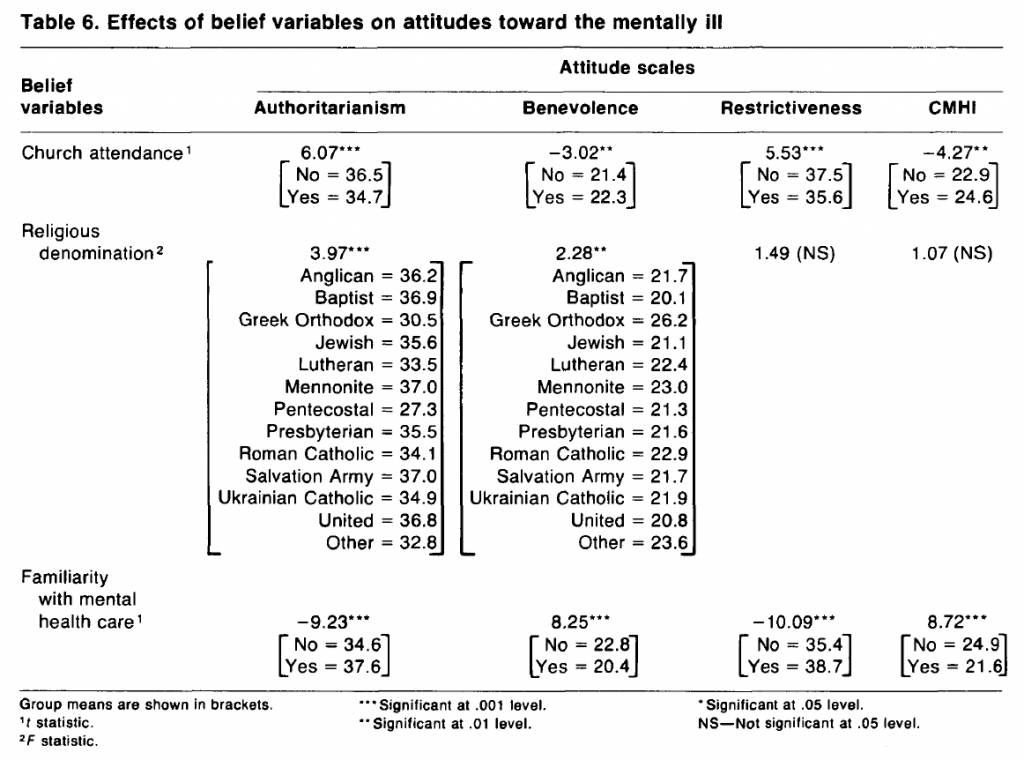
In terms of familiarity with mental health care, respondents who themselves had used mental health services or whose friends or relatives had used them expressed more sympathetic attitudes on all four scales. Personal experience of mental health care, whether direct or indirect, therefore has a significant effect on subsequent attitudes toward the mentally ill and the provision of mental health services.
Considered overall, the pattern of these relationships provides further support for the construct validity of the attitude scales. The relationships are consistent with the hypotheses derived from the underlying theoretical framework and are also similar to those reported in previous studies in which the personal correlates of attitudes toward the mentally ill have been examined. These results, however, go beyond those previously reported in that a broader range of personal characteristics was included in the analysis.
Attitudes Toward the Mentally Ill and Reactions to Mental Health Facilities. The relationship between attitudes toward the mentally ill and reactions to mental health facilities can be dealt with more briefly because we have discussed them in detail elsewhere (Taylor et al. 1979). The purpose of examining these relationships in the context of this article is to establish the predictive validity of the four scales.
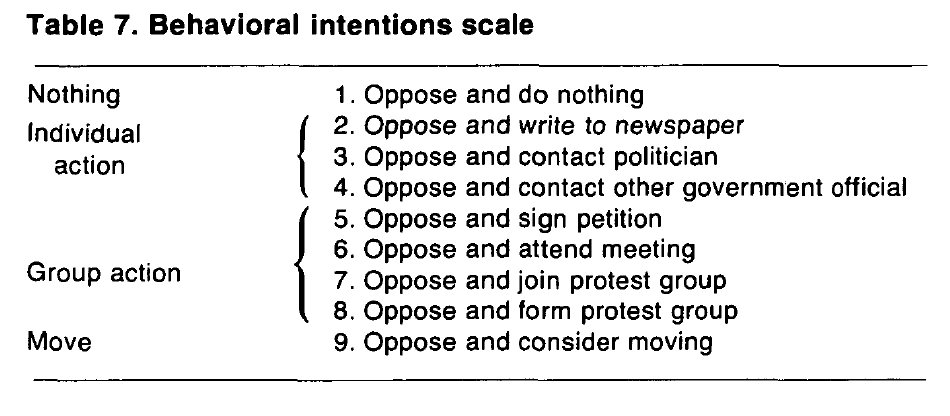
For this analysis, reactions to facilities were measured in both attitudinal and behavioral terms. All of the Toronto respondents (n = 1,090) rated the desirability of having a hypothetical facility located within three different distances of their home: within 1 block, 2 to 6 blocks, and 7 to 12 blocks. Ratings were on a 9-point labeled scale ranging from “extremely desirable” to “extremely undesirable.” For each facility-distance combination rated to any degree undesirable, respondents were asked what, if any, action they would most likely take in opposition. They were shown a list of nine possible actions (table 7). Respondents aware of an existing facility in their neighborhood were asked whether they were in favor of, opposed to, or indifferent toward it. If opposed, they were asked, using the same list, what actions they had taken. It is revealing that only 132 respondents were aware of a facility in their neighborhood, even through 384 were selected on the basis of living within a quarter mile of one.

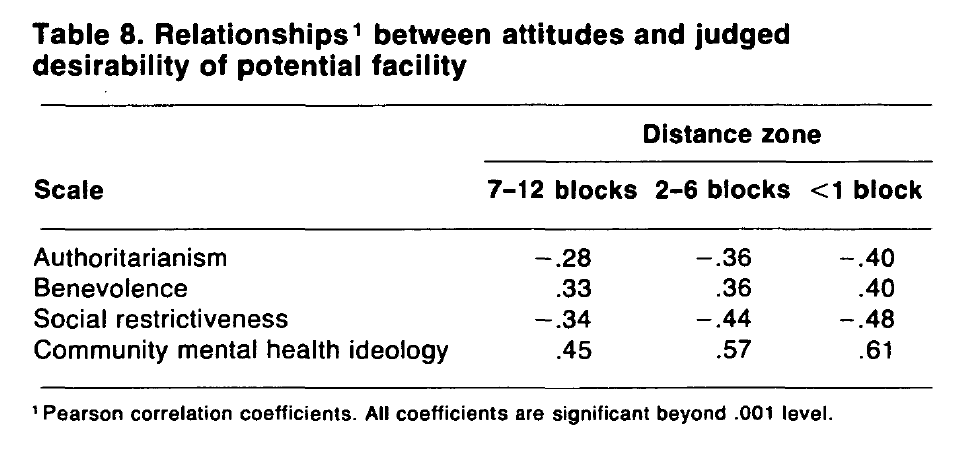
The general hypothesis that reactions to facilities are related to attitudes toward the mentally ill was tested first by correlating scores on the four scales with the facility desirability ratings for the three distance zones. The correlations (table 8) show highly significant relationships between all four scales and the three separate desirability ratings. Considered by attitude scale, the highest coefficient occurs for CMHI—the scale most directly concerned with community mental health. The positive sign of the coefficients for CMHI is consistent with the hypothesis that facility locations will be judged more desirable by those expressing pro-CMHI sentiments.
After CMHI, the scale most strongly correlated with the desirability ratings is social restrictiveness. This scale expresses the view that the mentally ill pose a threat to society and that their activities should therefore be closely controlled and supervised. Those holding a pro-social restrictiveness view would be predicted as judging neighborhood mental health facilities as undesirable, and this is confirmed by the negative signs of the coefficients. The coefficients for authoritarianism and benevolence are slightly lower, but their signs confirm the working hypotheses. Pro-authoritarian views are associated with less favorable ratings of facilities, and pro-benevolent sentiments coincide with more favorable ratings.
Considered by distance zone, the correlations again show a consistent pattern. For each scale, the coefficients increase with decreasing distance. This suggests that the variation in desirability ratings becomes increasingly systematic as the distance between facility and residence decreases. As a result, attitudes toward the mentally ill best predict the judged desirability of facility locations within a block of home.
For the analysis of relationships between attitudes toward the mentally ill and intended opposition to facilities, the nine possible actions were reduced to four categories: no action, individual action, group action, and consider moving (table 8). The pattern of the relationships from the analyses of variance (table 9) is similar to that just described for the desirability ratings. The relationships are strongest for CMHI and for the nearest distance zone. None of the four scales are significantly related to intended actions for the 7-12 block zone. For the other two zones, benevolence is the only scale that is not significantly related.
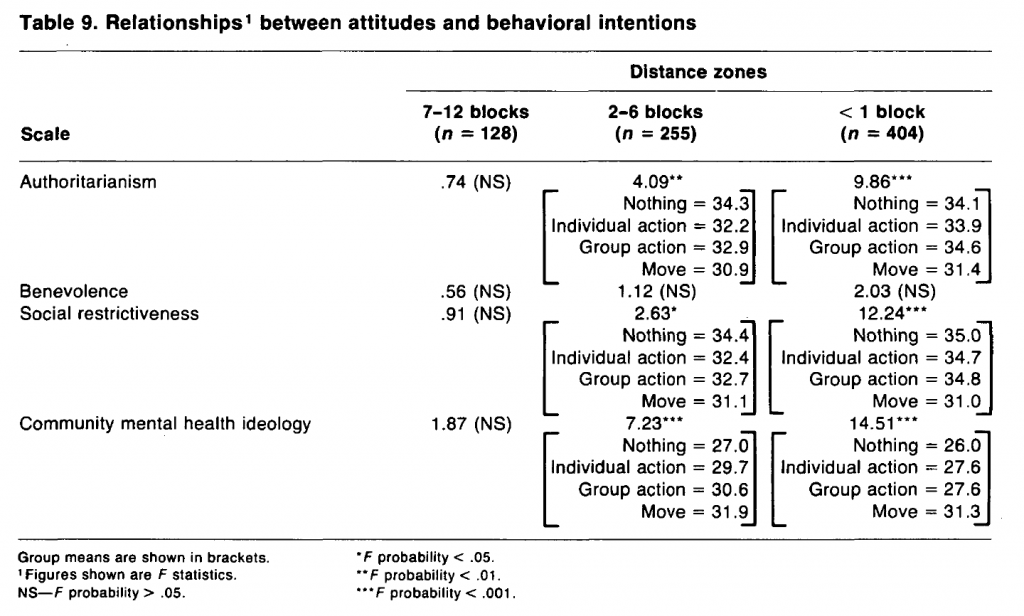
Examining the mean scale scores for the four categories of intended action reveals the pattern of the significant relationships. For example, in the case of the relationship with CMHI for the nearest distance zone, those intending no action are on average the most pro-CMHI, followed in order of describing community mental health orientation by those intending a group action, those intending an individual action, and those who would consider moving. The fact that the most community mental health oriented would do nothing, and the least so would consider moving, provides further support for the predictive validity of the CMHI scale. The ordering of the category means is equally consistent for the other two scales having significant relationships with intended action. For example, the category means on social restrictiveness, again for the nearest distance zone, show those who would consider moving as holding the most socially restrictive attitudes, followed by those intending individual action, group action, and no action—the exact reverse of the ordering observed for the CMHI scale.
A final analysis of variance was performed to test the relationships between the four attitude scales and attitudes toward existing facilities. The respondents who were aware of a facility (n = 132) were classified into three groups: in favor of (n = 95); indifferent toward (n = 19); and opposed to ( n =18). Mean scores on each of the attitude scales were significantly different for the three groups (table 10). Relationships are again strongest for CMHI followed by social restrictiveness, benevolence, and authoritarianism. For CMHI and benevolence, the highest mean scores are for the “in favor” group, and the lowest means are for the “opposed” group. The reverse holds for the authoritarianism and social restrictiveness scales.
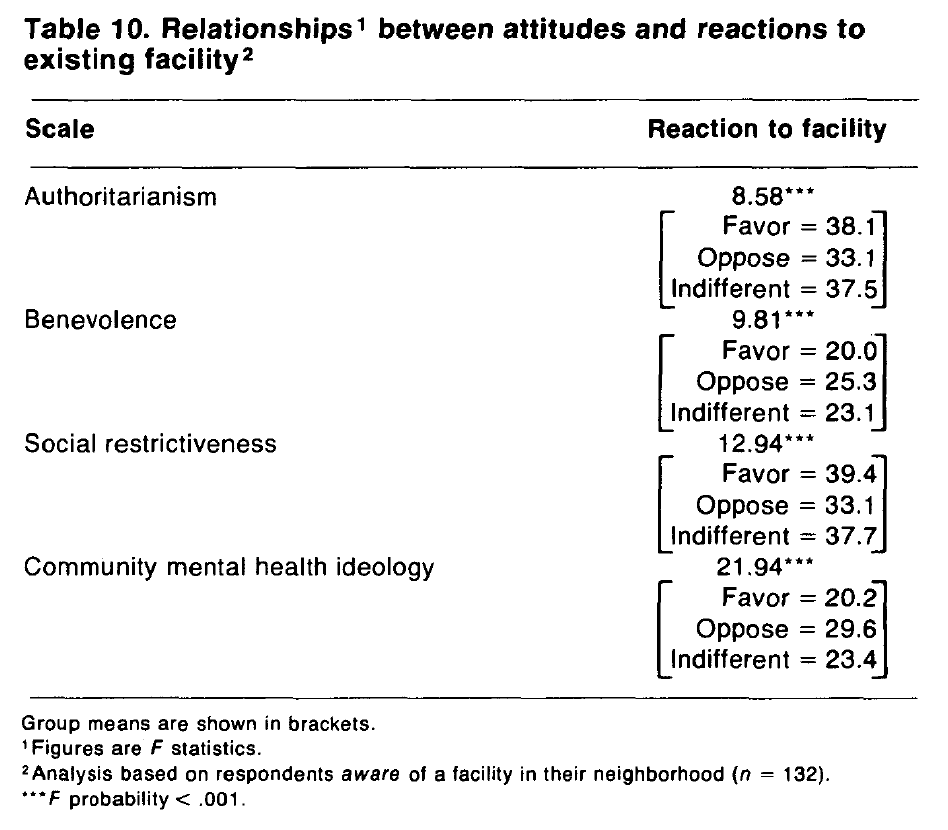

The strength, direction, and consistency of the relationships between the attitude scales and the different measures of response to hypothetical and existing mental health facilities provide strong evidence for the predictive validity of all four scales. For each of the response variables, the strongest validation occurs for the CMHI scale—a finding that is to be expected, and indeed hoped for, given the explicit community emphasis of this dimension of attitudes toward the mentally ill. Similarly, the repeated emergence of social restrictiveness as the second most powerful predictor is consistent with the content domain for that scale, which emphasizes the potential dangerousness of the mentally ill and the importance of maintaining social distance from them. The weaker predictive power for the benevolence scale, most apparent for the relationships with intended opposition to facilities, suggests a transcendent sympathetic attitude toward the mentally ill, which conceals important attitudinal variations exposed by the other scales. Taken together, these results are very encouraging not only in terms of scale validation but also in terms of their potential usefulness in future studies of community attitudes toward the mentally ill and mental health facilities.
Conclusions
In the Toronto study, the development of scales to measure community attitudes toward the mentally ill originated in the geographic problem of explaining spatial variations in public response to mental health facilities. Four existing scales were the basis for constructing a new set of scales representing the following four dimensions of community attitudes: authoritarianism, benevolence, social restrictiveness, and community mental health ideology. These scales differ from the originals in two main respects: first, by their emphasis on those facets of the content domain of each scale that relate most directly to community contact with the mentally ill; and second, by the statements’ being worded with a general public rather than professional sample in mind.
The internal and external validity of the CAMI scales was extensively analyzed using both the pretest and final data sets for the Toronto study. Weak items identified in the pretest were replaced before the major data collection phase. High levels of internal validity were shown for the final scales based on item-scale correlations, alpha coefficients, and factor analysis. External validity was examined in two ways within the theoretical framework for the Toronto study. Construct validity was assessed by analyzing relationships between the attitude scales and a range of personal characteristics. Predictive validity was tested by analyzing relationships between the scales and various measures of response to mental health facilities. In both cases, the strength, direction, and consistency of the relationships provided strong support for the external validity of the CAMI scales.
The theoretical and practical significance of the CAMI scales is well demonstrated in the Toronto study where these measures of attitudes toward the mentally ill are basic to the explanation and prediction of individual and community responses to mental health facilities (Dear and Taylor 1979). It remains for future studies to establish the applicability of the CAMI scales beyond the Toronto situation, although there is no a priori basis for questioning their generalizability.
The Toronto study is cross-sectional and provides no basis for establishing how sensitive the scales might be as indices of attitude change. It is planned to use the same scales in a study of community attitudes before and after the opening of a neighborhood mental health facility. This will introduce a longitudinal dimension whereby changes in attitude can be monitored and the usefulness of the scales for monitoring changes can be established.
The Toronto data provide only a limited basis for analyzing attitude-behavior relationships. As reported here, the scales are strongly related to behavioral intentions; the link with actual behavior remains uncertain, since so few of the Toronto respondents had actually taken any action to oppose a mental health facility. A focus for a future study is therefore to examine the predictive validity of the scales for actual behavior with respect to both the mentally ill and the mental health facilities.
The shift to community based mental health care emphasizes the need for reliable and valid methods for measuring public attitudes toward the mentally ill. The CAMI scales discussed in this article represent an attempt to develop such a method, and it is hoped that use of the scales in subsequent studies will further establish their validity. [1]
References
Adorno, T.W.; Frenkel-Brunswick, E.; Levinson, D.J.; and Sanford, R.N. The Authoritarian Personality. New York: Harper, 1950.
Baker, F., and Schulberg, H. The development of a community mental health ideology scale. Community Mental Health journal, 3:216- 225, 1967.
Boeckh, J.; Dear, M.J.; and Taylor, S.M. Property values and mental health facilities in Metropolitan Toronto. Canadian Geographer, 24:270-285, 1980.
Cohen, J., and Struening, E.L. Opinions about mental illness in the personnel of two large mental health hospitals. Journal of Abnor- 1 Copies of the statements are available on request from the authors. mal and Social Psychology, 64:349- 360, 1962.
Dear, M.J. Locational factors in the demand for mental health care. Economic Geography, 53(3):223-240, 1977a.
Dear, M.J. Psychiatric patients and the inner city. Annals of Association of American Geographers, 67:588- 594, 1977b.
Dear, M.J., and Taylor, S.M. Community Attitudes Toivard Neighbourhood Public Facilities. Report submitted to Social Science and Humanities Research Council of Canada, Ottawa, September 1979.
Fracchia, J.; Pintry, J.; Crovello, J.; Sheppard, C; and Merlis, S. Comparison of intercorrelations of scale scores from the opinions about mental illness scale. Psychological Reports, 30:149-150, 1972.
Giggs, J.A. The distribution of schizophrenics in Nottingham. Transactions, Institute of British Geographers, 59:55-76, 1973.
Gilbert, D.C., and Levinson, D.J. Ideology, personality and institutional policy in the mental hospital. Journal of Abnormal and Social Psychology, 53:263-271, 1956.
Gonen, A. “Community Support System for Mentally Handicapped Adults.” Regional Science Research Institute Discussion Paper 96, Philadelphia, 1977.
Holton, W.E.; Krame, B.M.; and New, P.K-M. Locational process: Guidelines for locating mental health services. Community Mental Health Journal, 9:270-280, 1973.
Joseph, A.E. The referral system as a modifier of distance decay effects in the utilization of mental health care. Canadian Geographer, 23 (2):159-169, 1979.
Miller, D.H. Community Mental Health: A Study of Services and Clients. Lexington, MA: Heath and Co., 1974.
Nunnally, J. Popular Conceptions of Mental Health: Their Development and Change. New York: Holt, Rinehart and Winston, Inc., 1961.
Nunnally, J. Psychometric Theory. New York: McGraw Hill, 1967.
Rabkin, J.G. Public attitudes toward mental illness: A review of the literature. Schizophrenia Bulletin, 1 (Experimental Issue No. 10):9-33, 1974.
Rabkin, J.G. “Determinants of Public Attitudes About Mental Illness: Summary of the Research Literature.” Presented at the National Institute of Mental Health Conference on Research on Stigma Toward the Mentally 111, Rockville, MD, January 24-25, 1980.
Segal, S.P., and Aviram, U. The Mentally 111 in Community-based Sheltered Care. New York: John Wiley & Sons, 1978.
Smith, C.J. Being mentally ill: In the asylum or the ghetto. Antipode, 7:53-59, 1975.
Smith, C.J. Distance and location of community mental health facilities: A divergent viewpoint. Economic Geography, 52:181-191, 1976.
Smith, C.J. “The Geography of Mental Health.” Washington, DC: Association of American Geographers Resource Paper, No. 76-4, 1977.
Taylor, S.M.; Dear, M.J.; and Hall, G.B. Attitudes toward the mentally iH and reactions to mental health facilities. Social Science and Medicine, 13D(4):281-290, 1979.
Trute, B., and Segal, S.P. Census tract predictors and the social integration of sheltered care residents. Social Psychiatry, 11:153-161, 1976.
White, A.N. Accessibility and public facility location. Economic Geography, 55(l):18-35, 1979.
Wolch, J.R. Residential location and the provision of human services: Some directions for geographic research. Professional Geographer, 31(3):271-277, 1979.
Wolpert, J. Social planning and the mentally and physically handicapped: The growing special service populations. In: Burchell, R.W., and Sternlieb, G., eds. Planning Theory in the 1980’s. New Brunswick, NJ: Center for Urban Policy Research, 1978. pp. 31-51.
Wolpert, ].; Dear, M.J.; and Crawford, R. Satellite mental health facilities. Annals of the Association of American Geographers, 65:24-35, 1975.
Wolpert, J., and Wolpert, E. The relocation of released mental hospital patients into residential communities. Policy Sciences, 7, 1976.
Acknowledgment
The research reported was supported by Grant No. 410-77-0322 of the Social Science and Humanities Research Council of Canada.
The Authors
Dr. S.M. Taylor holds a Ph.D. in geography from the University of British Columbia, and Dr. M.J. Dear, a Ph.D. in regional science from the University of Pennsylvania. Both are presently Associate Professors in the Department of Geography at McMaster University in Hamilton, Ontario, Canada.
Reprint requests should be sent to Dr. S.M. Taylor, Dept. of Geography, McMaster University, Hamilton, Ont., Canada L8S 4K1.
[1] Copies of the statements are available on request from the authors.
Save
Save